Mitochondria
Introduction to mitochondria
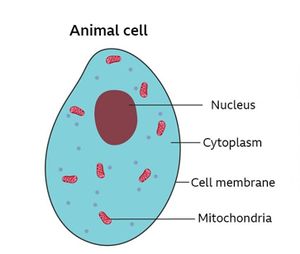
Basic biology teaches that cells are the "building blocks of life" but a cell has building blocks too. These cell building blocks include organelles (organelles literally means little organs). In animal cells, mitochondria are among those organelles. Mitochondria are found in every cell that has a nucleus. In the human body, that means mitochondria are present in every cell except red blood cells.
Mitochondria (the plural of mitochondrion) are often referred to as the “powerhouses of the cell” or “the energy factories of the cell.” They create energy for the cell, thus for our bodies. Think of mitochondria as the digestive system of a cell: they take in nutrients, break them down, and keep the cell full of energy.
The energy that mitochondria create is called adenosine triphosphate (ATP). Mitochondria make ATP through a sequence of reactions called the Krebs cycle, also known as the citric acid cycle or TCA cycle (tricarboxylic acid cycle). The final and perhaps most important step of this Krebs Cycle is called the electron transport chain where a majority of the ATP is created. Along with ATP, mitochondria also release byproducts like carbon dioxide, water, and free radicals. In moderation, free radicals can help us fight infection, but in excess they are injurious, they damage cell tissue and cause inflammation. ApoEε4s are already pro-inflammatory, so it’s in our best interest to keep free radical production, thus inflammation, down.
There are many mitochondria in the body, they make up 10% to 20% of the body by weight. Mitochondria are always working, at any given moment in time a person will only have 6 seconds of ATP left in the body. A person can go 3 days without water, but can’t go more than 6 seconds without ATP. That’s why cyanide is effective as a poison, it disrupts the electron transport chain of the mitochondria.
Mitochondria generate energy for the cell. Some cells need more energy than others, so those cells have more mitochondria. A cell can have hundreds to several thousand mitochondria depending on the function of the cell. The brain, heart, and retina have the most mitochondria and are the ones to suffer first when energy demand exceeds supply. Mitochondria lose their efficiency and become progressively dysfunctional with age. Mitochondrial dysfunction is a key factor in a myriad of diseases, including neurodegenerative and metabolic disorders.
The fundamental units of the brain and nervous system, neurons, require massive amounts of energy to function and can die if they don’t have a constant supply of ATP. To put things in perspective, the brain only makes up 3% of a body's weight, but it uses up 25% of the body's energy and it needs energy 24 hours a day. Anything that disrupts or impairs the brain’s ability to fuel itself has implications on cognition. The first priority of the mitochondria is to keep your cells oxygenized and blood pumping, in other words, basic survival, other functions such as cognitive thinking, is a secondary task, so cognition will suffer in order if mitochondria are unable to keep up with all their demands.
Degraded mitochondria is a hallmark of Alzheimer’s. Whether or not the poorly functioning mitochondria is causing Alzheimer’s is still under discussion, but regardless of if degraded mitochondria are causing, or a consequence, of Alzheimer’s, assuredly optimal mitochondria health sets the foundation for overall health and clear thought.
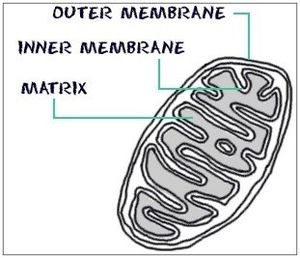
Mitochondria are shaped to maximize their energy production. They are made of two membranes: an outer membrane that cover the organelle, like a skin, and the inner membrane with multiple folds for increased surface area for chemical reactions to occur. Although typically represented as that bean-like shape in the accompanying graphic, mitochondria are very dynamic, they can change shape, interconnect like a power grid, travel within a cell (a neuronal axon can be a meter long, and mitochondria can travel from the cell body to the extreme end of the synapse where the energy is needed and then back), they can divide to increase their numbers, or fuse with other mitochondria, all to accommodate the needs of the cell.
It is thought that mitochondria descended from independent bacteria, so as organelles, they act a little different but they live symbiotically inside a cell now. Mitochondria have their own DNA and send DNA coded instructions to the nucleus of the cell and vice versa. While a cell has just one nucleus with one genome, there are many mitochondria in a cell each carry multiple genome copies and these copies vary within a cell. Within one person some mitochondria genomes might be healthy, but other defective, and different cells can have different proportions of affected mitochondria within them. In addition to producing ATP, mitochondria play other crucial roles including calcium homeostasis, metabolism, reactive oxygen species generation, apoptosis (determining which cells should die), intercellular communications, and stress responses.
Studies indicate that the E4 allele is more susceptible to mitochondrial dysfunction and there is at least one study that identified ApoE4 as more sensitive than E3s or E2s to the damaging free radicals that the mitochondria produce. Therefore it is advisable that ApoEε4s employ extra diligence in strategies to maximize the health of one’s mitochondria. How well your mitochondria function and age depend on three basic components:
- The mitochondria you inherited. Inheritance determines an individual's baseline mitochondrial function and durability. Mitochondrial DNA is inherited solely from the mother. This is why risk for Alzheimer’s Disease is higher in people who have a maternal history of it.
- What you’re exposing your mitochondria to that causes dysfunction, i.e. nutritional deficiencies, hormonal deficiencies, toxins, stress, etc.
- What you’re exposing your mitochondria to keep them running efficiently and/or making them stronger.
Strategies to improve (or reduce damaging) mitochondrial function
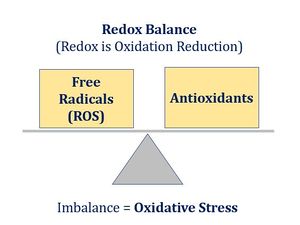
Our modern lifestyle and diets create a very damaging vicious circle of inflammation and oxidation. Most common disorders and diseases today are inflammation-oxidation based. When inflammation is initiated, it stimulates the production of highly destructive free radicals (molecules with unpaired electrons) called reactive oxygen species (ROS). When there is an imbalance between the amount of ROS and antioxidants in the body, the result is oxidative stress. Oxidative stress causes both genetic and mitochondrial damage, which in turn signals NF-κB ,the master protein that directs all inflammatory processes, to unleash an inflammatory cascade.
Oxidative stress is considered one of the main causes of modern diseases. It’s both the cause, as well as the result, of imbalanced oxidation.
Below are recommendations to help prevent mitochondrial damage and to improve mitochondrial function. This list is not all-inclusive.
Diet
Dr Bruce H. Cohen is a neurologist at Northeast Ohio Medical University and an expert in mitochondrial disease. As cited in this article The Care and Feeding of Your Mitochondria Cohen says that one of the chief reasons our mitochondria deteriorate is that we eat an excess of poor-quality foods and a deficit of healthy ones. The empty calories of sugars, flours, and other processed foods force mitochondria to burn through a great deal of junk — generating free radicals and inflammation as they go — before useful nutrients can be siphoned out. Unless we eat plenty of phytonutrients (natural chemicals that are found in plant foods), antioxidants (compounds that inhibit oxidation), healthy fats, proteins, and fiber, we aren’t giving our bodies the basic tools they need to repair the damage.
Dr Terry Wahls is another expert on mitochondria. She tells her personal inspirational story in this Tedx talk Minding your mitochondria. In short, Dr Wahls was diagnosed with multiple sclerosis (MS) in 2000. MS is a neurodegenerative disease and dysfunctional mitochondria play a role in neurodegenerative diseases. Her condition progressed such that she became confined to a tilt-recline wheelchair, a situation that lasted for four years. She sought out the best that conventional medicine had to offer, but it did very little. So she took matters into her own hands, relearned biochemistry, cellular physiology, and neuroimmunology, dove into available research, and connected with Functional Medicine. She restored her health, leaving her wheelchair by using a diet and lifestyle program she designed specifically for her brain. She is now dedicated to helping others restore their health. In addition to being a clinical professor and conducting clinical trials that test the effect of nutrition and lifestyle interventions to treat MS and other progressive health problems, she is also an author.
As Dr Wahls says in her book, The Wahls Protocol, “Cellular nutrition is everything. It is the very basis of health. It all comes down to the cell, because when the cells malfunction, eventually organs malfunction. When organs malfunction, eventually you malfunction."
Dr Wahls’s book outlines how she repaired her mitochondria. Wahls follows a diet similar to how our ancestors ate (Paleo). She recommends avoiding foods containing gluten, as well as dairy products, eggs, processed meats containing nitrates, and anything sweetened with sugar. Wahls also recommends avoiding all grains, legumes, peanuts, and soy. In addition to removing those foods, Wahls recommends eating nine cups of vegetables and fruits daily, including three greens (kale, collards, chard, lettuce-darker the better, etc), three deeply colored (beets, carrots, etc.), and three rich in sulfur (cauliflower, broccoli, cabbage, asparagus, brussel sprouts, turnips, radishes, onions, garlic, etc).
Dr Wahls is also familiar with the ApoE gene. You can listen to the ApoE4.info podcast with Dr Wahls here: Terry Wahls, MD: Heal Neurodegeneration w/ Paleo Principles
Foods to avoid that damage Mitochondria
(not an all inclusive list)
- Gluten. Even if you test negative for celiac disease, gluten causes inflammation. From neurologist Dr David Permutter’s book, The Grain Brain:
- Gluten isn’t just an issue for those with bona fide celiac disease,...Increasing numbers of studies are confirming the link between gluten sensitivity and neurological dysfunction. This is true even for people who have no problems digesting gluten and who test negative for gluten sensitivity.
- Dairy products. From Dave Asprey’s book Head Strong, (bold font added to emphasize effects on mitochondria):
- But even people who are not lactose intolerant are often sensitive to the main protein in dairy products, casein. Casein has a similar molecular structure to gluten, and people who are sensitive to one are often also sensitive to the other. In many people, casein breaks down into casomorphin, which binds to the opiate receptors in your brain and makes you feel sedated. Even worse, milk protein isolates are common ingredients in popular “keto” or “low-carb” protein bars. This is not what you want in a highly performing brain! Milk protein causes inflammation, which lowers mitochondrial function. Milk protein also binds to the good-for-you polyphenols in your diet (like the ones found in your coffee!) and makes them unavailable to your body—and your mitochondria. When you put milk protein isolates and casein into your coffee by adding milk, half-and-half, cream, or other creamers, the polyphenols become 3.4 times less absorbable in your body.4 The same thing happens if you use black coffee to wash down a milk protein–based “keto protein bar.” So not only does milk protein directly change your mitochondria for the worse, it also prevents you from absorbing the nutrients that can repair and strengthen your mitochondria.
- Vegetable oils. Oxidative stress in a bottle, that’s what Dr Catherine Shanahan, MD board certified Family Physician trained in biochemistry and genetics science, and author of three books on nutrition, calls vegetable oils (corn oil, soybean oil, safflower oil, cottonseed oil, sunflower oil, canola oil). In her interview by Naomi Whittel from 'The Real Skinny on Fat' documentary series, Dr Shanahan said (bold font added for emphasis):
- Cigarette smoking is bad for us because it promotes oxidative stress and oxidative stress is the great disease maker. But vegetable oils are oxidative stress in a bottle. And I've come out and said that if you have a choice between giving up your cigarette habit or your vegetable oil habit, keep the cigarettes because vegetable oil is worse for you. Cigarette smoking, you inhale it, your lungs get affected, your arteries get affected and some of the excretory pathways get hit heavy, but vegetable oil goes to every single cell in your body because every single cell has a membrane that has to be made out of fat and some of these fats are going to be the essential fats and they're going to be requesting this kind of stuff. And so your brain is built out of these polyunsaturated fatty acids. The lipoprotein circulating in your arteries have way too much of this stuff and they're all going to be susceptible to this kind of free radical cascade, the polymerization reaction that completely disrupts normal cellular function.
- Vegetable oils are easily replaceable with healthy oils such as olive oil, avocado oil, macadamia nut oil and others. Recognize that most restaurants, especially fast food restaurants, cook with damaging vegetable oils because they’re so cheap. (See Fats, Omega -3(ω-3) & -6(ω-6), DHA and More)
- Sugars. It takes more effort for the body to burn sugar than fat. Before the mitochondria can process sugars, they have to undergo a process called glycolysis, a sequence of ten enzyme-catalyzed reactions. This process causes more oxidative stress and creation of free radicals. Today’s modern diets consume a huge amount of sugars in comparison to amounts consumed from an evolutionary standpoint, our body has great difficulty coping with the amount of sugar it is currently being fed and we’re burning out our mitochondria with sugar. Don’t use artificial sweeteners instead, they’ve also been associated with increased reactive oxygen species. Keep sweets to a rare treat on special occasions.
- Transfats. Small amounts of trans fats are found naturally in meat and dairy. Artificial transfats were introduced in the 1950s in packaged foods, shortening, and margarine. Transfats cause inflammation and increases the damage to cell membranes and mitochondria. Evidence is limited, but trans fats from natural sources do appear to be less harmful than artificial ones. Artificial transfats offered a hardened source of fat with stability so foodstuffs such as cookies could be stocked in grocery stores and not turn greasy, mushy, or rancid over time. However, over time negative health effects became evident and in 2015, the US Food and Drug Administration (FDA) required elimination of trans fats from all food prepared in the United States by 18 June 2018. However according to 7 Foods That Still Contain Trans Fats products can still be distributed until January 2020, or in some cases 2021. Many other countries also have legal limits to trans fat content.
- Alcohol. Limit consumption or eliminate altogether, damaging to mitochondria.
- Non-organic foods. Foods sprayed with chemicals such as pesticides and insecticides increase oxidative stress.
- Fried foods/overcooked foods. High-temperature cooking, deep frying, grilling, and sautéing destroys nutrients and antioxidants in food thus making them more pro-inflammatory. Meat cooked at high temperatures create advanced glycation end products (AGEs) which contribute to increased oxidative stress [source: Advanced glycation end products, oxidative stress and diabetic nephropathy (Sho-ichi Yamagishi and Takanori Matsui, Mar-Apr 2010)]. Frying damages fats and makes them toxic. Even healthy fats can be damaged (oxidized) by cooking at high temperatures.
- Foods prone to hold mold toxins. Mold toxins are particularly toxic to your mitochondria. Avoid food products that are prone to hold mold toxins or go with quality products that are less likely to have mold toxins. Those most likely to hold mold toxins: coffee, dried fruit, wine, beer (gluten free, if you must), chocolate, nuts and corn.
Foods to add that help the Mitochondria
(not an all inclusive list)
- Fiber-rich foods. These help to detoxify the poisons that can build up when mitochondria slow down.
- Omega-3 fat. Omega-3 fat helps build mitochondrial membranes
- Organic produce. Whenever possible go with organic produce. Genetically modified organisms (GMOs) are commonly sprayed with pesticides that are highly toxic to mitochondria
- Phytonutrients. Phytonutrients (also known as phytochemicals) are natural chemicals found in plant foods. The best known phytonutrients are the carotenoids, flavonoids, polyphenols, indoles, lignans and isoflavones. Simply, eat a variety of fruits and vegetables, with a variety of colors/type, as recommended in the Wahls Protocol (see graphic above) because each class of phytonutrients has different effects. Different phytonutrients offer different benefits and often work synergistically when consumed together.
- Antioxidents. Antioxidents come from fruits, vegetables, herbs, spices, nuts, olives, chocolate, tea and wine. As the name suggests they oppose oxidation. Think of what happens to the inside of the apple when you cut it in half, it starts to turn brown from exposure to oxygen, that’s oxidation. But if you squeeze lemon juice on the apple, the browning stops, lemon juice is an antioxidant.
- There are thousands of antioxidents, but two well-known to be inhibitors of both inflammation and oxidative stress are quercetin and resveratrol.
- Quercetin Quercetin is a flavonoid that is both a free radical scavenger and anti-inflammatory. Found in highest concentration in capers, organically grown apples (green and wild apples are best for the lower sugar content) and onions. Other sources: bilberries, black currants, black elderberry, and lingonberries.
- Resveratrol: Resveratrol is a unique antioxidant because it can cross the blood-brain barrier. Resveratrol can increase glutathione levels (the potent antioxidant produced by the body) or prevent lipid oxidation. Resveratrol can be found in wine, don’t overdo it, alcohol is damaging to mitochondria and many wines have grapes that have been exposed to pesticides, the herbicide glyphosate, and a flame-retardant chemical is sometimes used in the wooden barrels and crates used to transport wine or grapes.
- The following lists: Types of Antioxidents and Antioxidant Rich Foods, were taken from Are Antioxidants Healthy, if you see a reference to a footnote, go to that website if you wish to investigate the footnote.
- Types of Antioxidants
- There are many different types of antioxidants that support the entire antioxidant system:
- *Vitamin A – A group of organic compounds like retinol, retinoic acid, and provitamin A carotenoids that are important for eyesight, proper growth, and the immune system.
- *Vitamin C or Ascorbic Acid – An essential nutrient required for tissue repair, immune system functioning, and production of some neurotransmitters[xv].
- *Vitamin E or α-Tocopherol – A group of eight fat-soluble compounds support the antioxidant system and control cell signaling.
- *Superoxide Dismutase (SOD) – An enzyme that neutralizes one of the main reactive oxygen species superoxide.
- *Catalase – An enzyme that catalyzes the decomposition of hydrogen peroxide into water and oxygen[xvi]. This protects against reactive oxygen species.
- *Glutathione – The body’s master antioxidant that protects cells against free radical damage, heavy metal toxicity, lipid peroxides, and oxidation[xvii].
- *Thioredoxin – A class of proteins that function as antioxidants and redox signallers by reducing oxidized proteins.
- *Carotenoids – Carotene protects plants against UV light and functions as an antioxidant. It gives carrots and sweet potatoes their orange color.
- *Ubiquinol (Coenzyme Q10) – A fat-soluble compound that helps to generate ATP and energy.
- *Alpha Lipoic Acid (ALA) – An organsulfur compound that is essential for aerobic metabolism. It’s also a co-factor for many enzyme systems like SOD.
- *Uric Acid – The most concentrated antioxidant in human blood that helps to mitigate oxidative stress, especially at high altitudes and under hypoxia[xviii].
- These antioxidants and enzymes require certain minerals to function properly like selenium, zinc, copper, manganese, magnesium, and vitamin D.
- There are many different types of antioxidants that support the entire antioxidant system:
- Types of Antioxidants
- Antioxidant Rich Foods
- Some antioxidants like glutathione can be synthesized by the body itself whereas others like vitamin C have to be obtained from dietary sources[xix].
- *Vitamin A Foods – Organ meat, liver, heart, fatty fish, salmon, whole eggs, carrots, dairy.
- *Vitamin C Foods – Citrus fruit, oranges, grapefruit, cruciferous vegetables, sauerkraut, berries.
- *Vitamin E Foods – Nuts, almonds, sunflower seeds, avocado, trout, seafood.
- *Glutathione Rich Foods – Sulfur rich foods like eggs, cruciferous, radishes, organ meats, beets, red meat, fish.
- *Carotenoid Foods – Carrots, sweet potatoes, seabuckthorn, tubers, some fruit like papaya, and melons.
- *CoQ10 Rich Foods – Organ meats, raw cacao, dark chocolate, seafood, meat, fish.
- *ALA Foods – Liver, beets, leafy greens, yams, potatoes.
- *Polyphenols are not necessarily antioxidants but they promote some antioxidant activity[xx].
- Some antioxidants like glutathione can be synthesized by the body itself whereas others like vitamin C have to be obtained from dietary sources[xix].
- Antioxidant Rich Foods
- It’s best to get your antioxidants from whole foods and focus on nutrient density rather than calories. For example, although papayas and melons have some vitamin C, but you’d get more antioxidants and less sugar from things like cruciferous vegetables and leafy greens.
Ketosis
Humans have two main fuels for energy: glucose (mostly from carbohydrates and sugar) and ketones (from burning fat). Today, with the modern western diet, people burn only glucose all the time. This is contrary to our evolutionary history when humans would often switch back and forth between glucose and fat (currently referred to as metabolic flexibility). Recently, there’s been a fair amount of “buzz” on lowering carbohydrate intake and adopting a ketogenic diet (eating in a manner such that the body uses fat as the primary source of fuel.) (See Ketosis and Ketogenic Diet). Some think of a ketogenic diet as strictly for weight loss, but it can be sustained in a manner that maintains weight stability. Adapting the body to easily make and use ketones promotes healthy mitochondria and healthy mitochondria benefits the brain, heart, and healthy aging.
Burning ketones is cleaner, more efficient, and produces more energy than burning glucose. When burning ketones, the mitochondria throw off fewer free radicals and create less oxidative stress (it’s like an engine that’s fed good gas, there’s fewer damaging emissions in the exhaust). It takes fewer steps to use ketones for energy over glucose, and with those fewer steps the mitochondria produce more ATP (energy for the cell) with ketones. Fat metabolism yields 48 ATP molecules from a fatty acid molecule versus a carbohydrate metabolism which yields 36 ATP molecules from a glucose molecule (continuing the engine analogy, it’s like getting more miles to the gallon with ketones).
Ketosis makes mitochondria stronger. In this study, Nutritional Ketosis and Mitohormesis: Potential Implications for Mitochondrial Function and Human Health (Vincent J Miller, et all 2018) the authors discuss how nutritional ketosis increases reliance on mitochondrial respiration and may induce mitohormesis (mitochondrial hormesis, i.e. a small amount of stress that results in healthier, stronger mitochondria, akin to using resistance training for stronger muscles). Additionally, this study identifies that besides being used to produce energy, the ketone known as beta hydroxy butyrate (BHB, also β-Hydroxybutyrate or βOHB) also acts as a signaling molecule, which is to say they transmit information between cells in your body thus presenting an additional benefit.
Ketosis also stimulates the production of more mitochondria in the cells. This is like adding more workers in the cell to produce energy. Sources: Mitochondrial biogenesis in the anticonvulsant mechanism of the ketogenic diet(Bough, K.J. et al, 2006) and The Ketogenic Diet: Uses in Epilepsy and other Neurologic Illnesses(KW Barañano and A L Hartman, 2008).
Fasting (Autophagy)
In his book The End of Alzheimer’s Dr Bredesen recommends ApoE4s fast 14 to 16 hours overnight. He writes:
- During sleep, our brain cells activate autophagy, the process of “self-eating” that recycles cellular components like damaged mitochondria and misfolded proteins, improving cellular health. Without autophagy, your cells would collect dysfunctional components – it would be like powering all your devices with worn-out batteries.
Intermittent fasting reduces the need for mitochondria to convert food to energy, thus reducing the production of free radicals. It also:
- Improves the activity of the electron transport chain and regulates the production of ROS and oxidative stress
- Supports mitochondrial quality control mechanisms, responsible for preventing and/or repairing damage
- Promotes the renewal of the mitochondrial network through the elimination of damaged mitochondria (autophagy) and the production of new mitochondria (biogenesis)
Proton Pump Inhibitors (Prilosec, Prevacid, Nexium, Losec)
We think proton pump inhibitors (PPIs) only effect the stomach, after all, they’re taken to help with conditions caused by excess stomach acid and they are effective in that regard.
But proton pumps aren’t limited to the stomach; they are present in every cell that has mitochondria, in other words every cell except red blood cells. The purpose of the mitochondria is to metabolize carbohydrates and fat to produce energy and they do that by pumping protons across the membrane to generate a source of electric potential that can form ATP. When proton pumps are inhibited, the mitochondria’s ability to generate energy is inhibited. From Proton Pump Inhibitors Kill Mitochondria And Brain Function :
- Essentially, PPIs kill mitochondria’s ability to produce energy in every cell in the body via their own proton pumps
Furthermore, according to Association of Proton Pump Inhibitors With Risk of Dementia (Willy Gomm et al, Apr 2016)
- ...some PPIs (eg, lansoprazole (Prevacid) and omeprazole (Prilosec and Losec)) have been reported to cross the blood-brain barrier where they are able to directly affect the brain.25,26
Also on PPIs:
Proton pump inhibitors and dementia: A nationwide population-based study (Nelsan Pourhadi et al, 5 Oct 2023) highlights from this study:
- After following 1,983,785 individuals for a median of 10 years, 99,384 developed dementia
- PPIs were used by 21.2% of cases and 18.9% of controls
- PPI use was associated with increased dementia rate regardless of time of treatment onset
- Magnitude of associations increased with younger age at diagnosis
- PPI use was not associated with dementia occurring after age 90 years
Regular proton pump inhibitor use and incident dementia: population-based cohort study (Peidong Zhang et al, 1 Sept 2022) from this paper:
- The finding of this large population-based cohort study indicates that the use of proton pump inhibitors is associated with an increased risk of incident dementia, particularly among APOE ε4 heterozygotes. (bold font added for emphaisis)
Proton pump inhibitors act with unprecedented potencies as inhibitors of the acetylcholine biosynthesizing enzyme—A plausible missing link for their association with incidence of dementia (Rajnish Kumar et al, 8 May 2020)
Is the Use of Proton-pump Inhibitors a Risk Factor for Alzheimer's Disease? Molecular Mechanisms and Clinical Implications (Kazuki Ide et al, 18 Nov 2018)
Statins
If you have been prescribed statins, don’t go off them without talking to your doctor. Before that conversation, you are advised to conduct additional research for a better understanding of the risk/benefit considerations.
From Statins and Mitochondrial Damage – Conclusion, Part 11 of 11:
- Research literature is now replete with reports of mitochondrial mutations associated with the aging process, many of the chronic diseases of aging, neurodegenerative diseases such as ALS and Parkinson disease and even many cases of autism.
- The underlying mechanism is oxidative damage - the consequence of energetic radicals on the adjacent mitochondrial DNA strands. Now we find that statins affect mitochondrial DNA in the same manner by their inhibition of both CoQ10 and dolichols. The end result is premature aging along with its often associated weakness, in coordination and faulty memory as well as increased numbers of neurodegenerative diseases.
Drugs that damage mitochondria or mitochondrial co-factors
If you have been prescribed any of the below drugs, don’t go off them without talking to your doctor. Before that conversation, you are advised to conduct additional research for a better understanding of the risk/benefit considerations.
Drugs that interfere with Coenzyme Q10 (CoQ10)
Coenzyme Q10 (CoQ10), or ubiquitol is very important to mitochondrial function. According to Coenzyme-Q10-(CoQ10)-and-Mitochondrial-Function Coenzyme Q10 (CoQ10) and Mitochondrial Function effective mitochondrial function relies on a number of things but CoQ10 is of particular interest because it not only supports the mitochondrial respiratory chain, but also acts as a powerful antioxidant in mitochondrial membranes. Additionally, CoQ10 concentrates in the same organs that have the highest mitochondrial density.
CoQ10 is difficult to get into your diet and we get far less efficient at producing CoQ10 after age 50. But CoQ10 protects our cells from oxidative stress and damage. Plus it aids in the production of energy by our cells.
Some of the medications that interfere with coenzyme Q include, as taken from Dr Wahls book, The Wahls Protocol:
- Tricyclic antidepressants
- Benzodiazepines
- Sulfonylureas
- Thiazide diuretics
- Beta blockers
- Acetaminophen (Tylenol)
Drugs that interfere with B vitamins
B vitamins play an essential role in maintaining mitochondrial function. The following are medications that interfere with B vitamin absorption as taken from Dr Wahls book, The Wahls Protocol:
- Diuretics
- Metformin and other common diabetic medications
- Birth control pills
- Medications that lower stomach acid
- Certain antibiotics
- Benzodiazepines
- Tricyclic antidepressants
- NSAIDS (nonsteroidal anti-inflammatory drugs, such as ibuprofen)
- Aspirin
- Proton pump inhibitors
Other Drug Considerations
From Dr Bredesen’s book, The End of Alzheimer’s:
- Since many chemicals damage mitochondria, it is helpful to know whether you have been exposed to these, especially in significant amounts or over a long period of time. The list includes antibiotics (which kill bacteria, and thus can be toxic to our mitochondria since they are descendants of bacteria), statins, alcohol, L-DOPA (prescribed to treat Parkinson’s disease), griseofulvin (prescribed for fungal infections), acetaminophen (Tylenol), NSAIDs (aspirin, ibuprofen, and related drugs), cocaine, methamphetamine, or AZT (azidothymidine, used for viral infections including HIV/ AIDS).
Chronic Stress
Being constantly stressed and inflamed promotes oxidative stress and excess cortisol, which in turn leads to mitochondrial damage and disease. Your job and finances aren’t the only sources of stress, sometimes it comes from sources we never suspected. (See Stress)
Exercise
Exercise can be beneficial by increasing the number of mitochondria and the body’s manufacture of antioxidents. But there is such a thing as too much exercise which will produce damaging excess oxidative stress. (See Exercise - Types, Lengths, and Benefits)
When you say the word “exercise” to some people they respond negatively, but it doesn’t have to be a “butt-kicking” exhausting drudgery. Exercise comes in various forms. When it comes to cardiovascular exertion, there are 5 “zones” representing a rating of perceived exertion. These zones start with Very Light exertion (zone 1) to Very Hard (zone 5). Zone 2 aka “Light” is prolonged low-intensity aerobic training. It is of particular interest to those wishing boost their mitochondria. Zone 2 exercise stimulates your mitochondria the most to create ATP and improves mitochondrial efficiency. See Stay Fit, Stay Young: Mitochondria in Movement: The Role of Exercise in the New Mitochondrial Paradigm(Jesus R. Huertas et al, 19 Jun 2019)
Zone 2 offers many other health benefits also: increased cardiovascular health, helpful if trying to lose weight, improves mood, and prevents injury.
Zone 2 cardio is an exercise performed within a heart rate zone that represents 60% to 70% of the maximum heart rate (MHR). To determine whether you're in zone 2, you can go off perceived exertion or calculate your maximum heart rate and calculate a target range from there.
Most will tell you that your maximum heart rate is found using the equation: 220 - your age = MHR. (So if 60 years old: 220 – 60 = 160 maximum heart rate (MHR). Then 60% to 70% of that MHR is a Zone 2 heart rate target of 96 to 112.
However, a newer formula used among trainers is 208 - (0.7 x your age) = MHR. (So if 60 years old: 208 – (0.7x60 which is 42) = 166. Then 60 to 70% of 166 is a Zone 2 heart rate target of 99.6 to 116.2.)
There is no clear consensus on the amount of time zone 2 training, however, at least 30 minutes to it two to three times per week is a good recommendation.
Cigarette smoke, marijuana smoke, and second hand smoke
Smoking cigarettes even being in the presence of smoke causes oxidative stress and increases free radicals, reference: Smoking and oxidative stress
This also applies to smoking marijuana. Reference: Oxidative Stress Produced by Marijuana Smoke An Adverse Effect Enhanced by Cannabinoids
Sleep
Sleep deprivation and circadian mismatches cause oxidative stress which damages the mitochondria. Blue light exposure from modern electronic devices and energy saving light sources also disrupts your sleep. (See Circadian Rhythm for more info on blue light and how it disrupts sleep. Also see Sleep)
Heat and Cold exposure
Cold exposure in the form of cold showers or cryotherapy can boost mitochondria.
Heat, such as from a sauna, acts as a mild stress signal and triggers a beneficial adaptive response in mitochondria that increase their functional capacity.
Photobiomodulation aka Low Level Laser Therapy
Photobiomodulation (PBM) is light therapy using sources that include lasers, light emitting diodes, and/or broadband light, in the visible (400 – 700 nm) and near-infrared (700 – 1100 nm) electromagnetic spectrum. PBM is the term being used more frequently now for what is also known as Laser Therapy or Low Level Laser Therapy (LLLT).
It is proposed that the low level visible red to near infrared light (NIR) energy is absorbed by mitochondria and converted into ATP for cellular use. PBM is also helpful in forming EZ water (read next).
EZ water
Dr Gerald Pollack, bioengineering professor and editor of the scientific journal Water discovered a phase of water that is not liquid, gas, or solid, but a fourth phase of water that is called exclusion zone water or EZ water.
Since our cells are two-thirds water by volume, the amount and type of water in your cells is incredibly important. Regular water is neither positively or negatively charged. EZ water is negatively charged and therefore facilitates cellular function. The more negative the charge, the better your cells are able to function. Oxidation causes cells to lose their negative charge and impairs function.
In Dr Pollack's lab they conducted an experiment where they flowed water through a narrow tube. Then they exposed water to UV light to create EZ water and the water flowed through the tube 5 times faster. EZ water helps lymphatic flow, the lymph system is what removes toxins and waste products in your body. Without proper lymphatic flow, chronic damaging inflammation will result.
EZ water is also particularly critical to mitochondrial function for neuronal communication. Specifically, there’s a cell structure called microtubules that are a key part of shuffling mitochondria around in neurons. EZ water helps the movement of mitochondria in these microtubules as well as providing the neurons the negative charge that is essential to sending a signal to communicate.
You get EZ water when you drink raw vegetable juices, fresh spring water, or glacial meltwater, and it forms spontaneously when regular water is exposed to infrared light or vibration. EZ water forms in your cells when you expose your skin and eyes to unfiltered sunlight for a few minutes every day without sunglasses, or clothing or sunscreen. Photobiomodulation (low-level light therapy) and infrared saunas help with create EZ water in the body. Earthing, also known as grounding, a practice where you connect with the earth by walking barefoot outside outdoors on natural earth surfaces or indoor with an earthing product also helps the body build up negative charges and build more EZ water.
How to test for mitochondrial function
Unfortunately, there is no simple blood test to test for mitochondrial function. There are indirect tests: organic acids, breath tests nuclear magnetic resonance test, mitochondrial DNA sequencing, and muscle biopsies.
A deeper Dive into the science: Mitochondria and ApoEε4 health concerns
The three primary health conditions that effect ApoEε4s are: Alzheimer’s Disease, Cardiovascular Disease, and shortened longevity. The following are some research findings of how mitochondria affect those conditions.
Alzheimer’s Disease and Brain Health
The Mitochondrial Cascade Hypothesis
In 2004, when the amyloid cascade hypothesis was popular, neurology researchers Dr Russell Swerdlow and Shaharyar Khan, PhD, proposed the mitochondrial cascade hypothesis in A “mitochondrial cascade hypothesis" for sporadic Alzheimer's disease(RH Swerdlow and SM Khan, 2004). They recognized holes in the current thought, specifically in what initiated the most common form of Alzheimer’s Disease, the late-onset, sporadic form. They proposed it starts with the mitochondria and that:

- What a person inherits sets the baseline for the mitochondrial electron transport chain’s production of reactive-oxygen species (ROS). Reactive oxygen species are free radicals, they can cause damage to DNA, RNA, and proteins, and may cause cell death. That baseline sets the pace for mitochondrial damage accumulation.
- That inherited and environmental factors influence the durability of the mitochondria thus how they age and change. Greater mitochondrial durability associates with slower brain aging and lesser mitochondrial durability associates with faster brain aging
- When changes to the mitochondria passes a certain threshold, cognitive symptoms ensue.
In other words, when damaging insults occurs, the body responds to address them, when the mitochondria are strong enough to hold the damage in check, the result is innocuous, but when the insults are too great and/or the mitochondria too weak to deal with the insults, the damage snowballs and the eventual result is Alzheimer’s.
In 2009, Swerdlow and Khan published an update to their hypothesis in The Alzheimer's disease mitochondrial cascade hypothesis: an update.(Swerdlow and Khan, 2009)
In 2010, the hypothesis was updated with: The Alzheimer's Disease Mitochondrial Cascade Hypothesis ((Russell H. Swerdlow, et al, 2010)
- Since then [2004, the initial publication] several lines of investigation report data consistent with or supportive of our hypothesis.
Regarding how ApoE influences the Mitochondrial Cascade hypothesis from this 2010 paper:
- Although late-onset AD is considered a sporadic or pseudo-sporadic disorder it is clear that AD risk is genetically influenced. In 1991 an association between AD and the proximal long arm of chromosome 19 was revealed [94]. Polymorphisms in the APOE gene are believed to mediate this association but the physiologic basis of this relationship remains uncertain [95]. Different studies report different potential mechanisms. Apolipoprotein E protein has been shown to influence Aβ trafficking and cell signal transduction, either of which could affect Aβ toxicity [96, 97]. Apolipoprotein E or its degradation products also appear to influence mitochondrial function [98]. A recent study of autopsy brains from young individuals found APOE4 carriers had reduced posterior cingulate cortex cytochrome oxidase activity [88].
Most recently, their findings were updated in The Alzheimer's disease mitochondrial cascade hypothesis: progress and perspectives. (Russell H. Swerdlow, et al, 2014) and From their conclusion (boldface added for emphasis):
- The mitochondrial cascade hypothesis sees Aβ as a marker of brain aging, and not AD's singular cause. Because of this, we would not solely equate the presence of brain Aβ changes with the presence of AD, and we would not universally consider the Aβ deposition process as a disease process. According to our hypothesis, Aβ marks a continuum between brain aging and AD, as opposed to a unique and age-unrelated event. In some ways, therefore, brain aging and LOAD [Late Onset Alzheimer’s Disease] also represent a continuum.
- The mitochondrial cascade hypothesis proposes changes in mitochondrial function change Aβ homeostasis. Early on, these mitochondrial changes increase Aβ production and cause it to accumulate. Later on, as mitochondrial dysfunction surpasses a threshold Aβ production and accumulation declines.
- According to our hypothesis, arresting brain aging will arrest both the development and progression of AD. We believe manipulating mitochondrial function and cell bioenergetic pathways will ultimately achieve this goal.
Other research on mitochondria and Alzheimer’s Disease
Enhanced mitochondrial fusion during a critical period of synaptic plasticity in adult-born neurons(Sandra M.V. Kochan et al, 5 Apr 2024) From this paper, researchers made a groundbreaking discovery about the critical role of mitochondrial fusion in the maturation process of adult-born neurons in the brain. Their study shows that as neurons develop, their mitochondria undergo dynamic changes that are crucial for the neurons’ ability to form and refine connections, supporting synaptic plasticity in the adult hippocampus. This insight opens new avenues for understanding and potentially treating conditions like Alzheimer’s and Parkinson’s by targeting mitochondrial dynamics to enhance brain repair and cognitive functions.
Mitochondria in Alzheimer’s Disease Pathogenesis (Reiss, A.B et al, 30 Jan 2024)
- Mitochondria are an essential organelle involved in cellular bioenergetics and signaling pathways. Mitochondrial processes crucial for synaptic activity such as mitophagy, mitochondrial trafficking, mitochondrial fission, and mitochondrial fusion are dysregulated in the AD brain. Excess fission and fragmentation yield mitochondria with low energy production. Reduced glucose metabolism is also observed in the AD brain with a hypometabolic state, particularly in the temporo-parietal brain regions. This review addresses the multiple ways in which abnormal mitochondrial structure and function contribute to AD. Disruption of the electron transport chain and ATP production are particularly neurotoxic because brain cells have disproportionately high energy demands. In addition, oxidative stress, which is extremely damaging to nerve cells, rises dramatically with mitochondrial dyshomeostasis. Restoring mitochondrial health may be a viable approach to AD treatment.
Decoding metabolic signatures in Alzheimer’s disease: a mitochondrial perspective(Daniele Bano et al, 1 Dec 2023)
- ...there is a substantial body of evidence suggesting that hypometabolism occurs in the brains of individuals at the prodromal stage before dementia is diagnosed, which may reflect an early role of metabolic dysfunction in AD. This perspective surveys the vast literature and critically assesses the current evidence demonstrating a mitochondrial contribution to AD. Additionally, we discuss our interpretations of the reported mitochondrial signatures and consider how altered mitochondrial bioenergetics may be an additional risk factor for AD pathogenesis.
Mitochondrial DNA and Inflammation in Alzheimer’s Disease (Giacoma Galizzi and Marta Di Carlo, 25 Oct 2023)
- Mitochondrial dysfunction and neuroinflammation are implicated in the pathogenesis of most neurodegenerative diseases, such as Alzheimer’s disease (AD). In fact, although a growing number of studies show crosstalk between these two processes, there remain numerous gaps in our knowledge of the mechanisms involved, which requires further clarification. ... This review of works published in recent years is focused on the description of the mitochondrial contribution to neuroinflammation and neurodegeneration, with particular attention to mitochondrial DNA (mtDNA) and AD.
Exercise and mitochondrial remodeling to prevent age-related neurodegeneration(Colleen L. O’Reilly et al, 9 Jan 2023)
- “This mini-review describes the role of mitochondria in neurodegeneration and brain health, current practices for assessing both aspects of mitochondrial remodeling, and how exercise mitigates the adverse effects of aging in the brain. Exercise training elicits functional adaptations to improve brain health, and current literature strongly suggests that mitochondrial remodeling plays a vital role in these positive adaptations. Despite substantial implications that the two aspects of mitochondrial remodeling are interdependent, very few investigations have simultaneously measured mitochondrial dynamics and protein synthesis. An improved understanding of the partnership between mitochondrial protein turnover and mitochondrial dynamics will provide a better understanding of their role in both brain health and disease, as well as how they induce protection following exercise.”
Relationship between Cognitive Dysfunction and Age-Related Variability in Oxidative Markers in Isolated Mitochondria of Alzheimer’s Disease Transgenic Mouse Brains (Naoki Yoshida, et al, 26 January 2022)
- These results indicate that oxidative stress in the hippocampi of AD mice is high compared to other brain regions and may induce mitochondrial dysfunction via oxidative damage. Protection of mitochondria from oxidative damage may be important to maintain cognitive function.
Mitochondrial Dysfunction as a Driver of Cognitive Impairment in Alzheimer’s Disease (Chanchal Sharma et al, 3 May 2021)
- We present an overview of the importance of mitochondria for maintenance of neuronal function and how mitochondrial dysfunction acts as a driver of cognitive impairment in AD. Additionally, we provide a brief summary of possible treatments targeting mitochondrial dysfunction as therapeutic approaches for AD.
Mitochondrial Functioning and the Relations among Health, Cognition, and Aging: Where Cell Biology Meets Cognitive Science (David Geary, 30 Mar 2021)
- Mitochondrial functions, including cellular energy production and control of oxidative stress, among others, are well situated to explain the relations among the brain, cognition, and health. Here, I provide an overview of the relations among cognitive abilities, associated brain networks, and the importance of mitochondrial energy production for their functioning. These are then linked to the relations between cognition, health, and aging. The discussion closes with implications for better integrating research in cognitive science and cell biology in the context of developing more sensitive measures of age- and disease-related declines in cognition.
Mitochondrial Dysfunction and Oxidative Stress in Alzheimer’s Disease (Afzal Misrani et al, 18 Feb 2021)
- Mitochondria play a pivotal role in bioenergetics and respiratory functions, which are essential for the numerous biochemical processes underpinning cell viability. Mitochondrial morphology changes rapidly in response to external insults and changes in metabolic status via fission and fusion processes (so-called mitochondrial dynamics) that maintain mitochondrial quality and homeostasis. Damaged mitochondria are removed by a process known as mitophagy, which involves their degradation by a specific autophagosomal pathway. Over the last few years, remarkable efforts have been made to investigate the impact on the pathogenesis of Alzheimer’s disease (AD) of various forms of mitochondrial dysfunction, such as excessive reactive oxygen species (ROS) production, mitochondrial Ca2+ dyshomeostasis, loss of ATP, and defects in mitochondrial dynamics and transport, and mitophagy. Recent research suggests that restoration of mitochondrial function by physical exercise, an antioxidant diet, or therapeutic approaches can delay the onset and slow the progression of AD. In this review, we focus on recent progress that highlights the crucial role of alterations in mitochondrial function and oxidative stress in the pathogenesis of AD, emphasizing a framework of existing and potential therapeutic approaches.
Mitochondrial Dysfunction in Alzheimer’s Disease: A Biomarker of the Future? (Simon M. Bell et al, 11 Jan 2021)
- The function of mitochondria in both the nervous system and rest of the body is altered early in this [Alzheimer’s] disease, and both amyloid and tau have detrimental effects on mitochondrial function. In this review article, we describe how the function and structure of mitochondria change in AD. This review summarises current imaging techniques that use surrogate markers of mitochondrial function in both research and clinical practice, but also how mitochondrial functions such as ATP production, calcium homeostasis, mitophagy and reactive oxygen species production are affected in AD mitochondria. The evidence reviewed suggests that the measurement of mitochondrial function may be developed into a future biomarker for early AD.
This news release Healthy mitochondria could stop Alzheimer's is reporting on the findings of a paper Enhancing mitochondrial proteostasis reduces amyloid-β proteotoxicity(Vincenzo Sorrentino et al, Dec 6, 2017) but that paper is behind a paywall, so from the news release (boldface added for emphasis):
- Using a bioinformatics and experimental approach, scientists have found that rendering mitochondria resistant to damage can halt diseases caused by amyloid toxicity, such as Alzheimer's disease.
From another paper, also behind a paywall, Mitochondrial dysfunction: the missing link between aging and sporadic Alzheimer's disease (Amandine Grimm et al, April 2016) the abstract cites (boldface added for emphasis):
- In the present review, we compare the common features observed in both brain aging and AD, placing mitochondrial in the center of pathological events that separate normal and pathological aging. We emphasize a bioenergetic model for AD including the inverse Warburg hypothesis which postulates that AD is a consequence of mitochondrial deregulation leading to metabolic reprogramming as an initial attempt to maintain neuronal integrity.
Without the barrier of a paywall, this paper offers much valuable information. Mitochondrial Dysfunction in Alzheimer’s Disease and the Rationale for Bioenergetics Based Therapies(Isaac G. Onyango, et al, 2016) (boldface added for emphasis):
- While the molecular basis underlying this multifactorial neurodegenerative disorder remains a significant challenge, mitochondrial dysfunction appears to be a critical factor in the pathogenesis of this disease. It is therefore important to target mitochondrial dysfunction in the prodromal phase [the onset of a disease before specific signs and symptoms develop] of AD to slow or prevent the neurodegenerative process and restore neuronal function.
- In this review, we discuss mechanisms of action and translational potential of current mitochondrial and bioenergetic therapeutics for AD including: mitochondrial enhancers to potentiate energy production; antioxidants to scavenge reactive oxygen species and reduce oxidative damage; glucose metabolism and substrate supply; and candidates that target apoptotic and mitophagy pathways to remove damaged mitochondria.
- AD brain mitochondria have reduced membrane potential, increased permeability, and produce excess reactive oxygen species (ROS) which damages proteins, lipids, and nucleic acids, and are believed to contribute to the pathogenesis of neurodegeneration. Growing evidence suggest that elevated amyloid-β (Aβ) levels contribute to the mitochondrial abnormalities and although the mechanism is not clearly established, both amyloid precursor protein (APP) and Aβ are found in mitochondrial membranes and interact with mitochondrial proteins. Overproduction of the APP and Aβ may affect dynamics of mitochondrial fusion/fission [12-14], impair mitochondrial transport, disrupt the electron transfer chain, increase ROS production [15-17], and impair mitochondrial function [18-20]. These findings build a strong case for mitochondrial dysfunction in AD and effective treatment will likely include targets that address mitochondrial function [21-23].
- Conclusion: Mitochondrial function is deregulated in AD and there is growing interest in understanding how altered mitochondrial function may be targeted to inhibit neurodegeneration. Proper modulation of mitochondrial turnover overall to eliminate dysfunctional mitochondria while maintaining efficient functional mitochondrial mass in response to stresses, including hypoxia and nutrient starvation may be relevant in delaying or managing the degenerative process in aging and AD. By preventing the generation of excessive ROS and conserving valuable nutrients neuronal survival may be promoted under conditions of energetic stress
In recognizing that mitochondrial dysfunction is one of the earliest and most prominent features of Alzheimer’s Disease, but not convinced that it is the root cause of the disease, the authors of this paper Alzheimer's disease diverse aspects of mitochondrial malfunctioning (Renato X Santos et al, 2010) reviewed physiological mitochondrial function, the importance of organelle dynamics and mitophagy (mitochondrial autophagy), and the mitochondrial pathophysiological alterations that occur in Alzheimer’s and in the conclusion wrote (boldface added for emphasis):
- Although AD etiogenesis is largely unknown, it is constantly growing in intricacy. Aβ and tau pathology are the most studied histopathological markers and considered by many authors as the cause of disease, particularly of genetic origin. Aβ and tau are unlikely causes of the sporadic, late onset form of AD, with mitochondria instead assuming a central stage, since these organelles are known to lose efficiency and progressively become dysfunctional with age, which is correlated with increased ROS production. Mitochondrial function has been shown to be impaired in AD in terms of metabolic energetic production and regulation of the levels of second messengers (ROS, Ca2+), partially due to either accumulated damage to mtDNA or the direct harmful effects of oxidative stress or Aβ on mitochondrial components. Also mitochondrial dynamics has been documented to be altered in AD. Indeed, mitochondrial trafficking disruption in AD potentially compromises normal neurophysiological functions, such as neurotransmission. Moreover, mitochondrial fission/fusion and mitophagy disruption may have consequences on the maintenance of the homogeneity and a healthy cellular mitochondrial pool. In short, mitochondrial malfunctioning is one most likely major cause of onset and neurodegeneration in sporadic AD brains.
In this paper (behind a paywall) Brain mitochondria as a primary target in the development of treatment strategies for Alzheimer disease (Aliev G, et al, 2009) The researchers suggest that it is constricted blood flow that induces oxidative stress and over time that is what initiates the mitochondrial failure that leads to Alzheimer’s Disease. From the abstract:
- We summarize the large body of evidence which indicates that sporadic, late-onset AD results from a vascular etiology by briefly reviewing mitochondrial damage and vascular risk factors associated with the disease and then we discuss the cerebral microvascular changes reason for the energy failure that occurs in normal aging and, to a much greater extent, AD.
From Mitochondria, Cognitive Impairment, and Alzheimer's Disease(M. Mancuso, et al, 2009) the abstract states (boldface added for emphasis):
- To date, the beta amyloid (Aβ) cascade hypothesis remains the main pathogenetic model of Alzheimer's disease (AD), but its role in the majority of sporadic AD cases is unclear. The “mitochondrial cascade hypothesis” could explain many of the biochemical, genetic, and pathological features of sporadic AD. Somatic mutations in mitochondrial DNA (mtDNA) could cause energy failure, increased oxidative stress, and accumulation of Aβ, which in a vicious cycle reinforce the mtDNA damage and the oxidative stress. Despite the evidence of mitochondrial dysfunction in AD, no causative mutations in the mtDNA have been detected so far. Indeed, results of studies on the role of mtDNA haplogroups in AD are controversial. In this review we discuss the role of the mitochondria, and especially of the mtDNA, in the cascade of events leading to neurodegeneration, dementia, and AD.
Neurons are extremely sensitive to attacks by destructive free radicals and according to this paper, Oxidative stress and Alzheimer disease (Yves Christen, Feb 2000) APOE is also sensitive to attacks by free radicals, with E4 being more sensitive than E3s or E2s. As stated in this paper:
- The E4 allele of apo E has been linked to both late-onset family forms and sporadic forms of AD, whereas the E2 allele appears to offer protection. This discovery inspired many new research projects and working hypotheses suggesting that oxidative processes play a role in AD. Apo E helps transport cholesterol through both the vascular system and the neurons. In the brain, apo E is the crucial cholesterol carrier, which explains the role it plays in neuroplasticity-related phenomena because these require changes to membrane lipids and, therefore, a cholesterol-dependent function. Poirier (80) maintains that apo E has a beneficial effect for neuronal protection but that the apo E4 isoform is less effective than are the apo E2 and E3 isoforms. (In other words, apo E4 may not be toxic, but simply capable of producing a less-favorable effect.) Miyata and Smith (81) showed that apo E has a beneficial effect against free radicals. Apo E reduced neuronal death caused by hydrogen peroxide and β-amyloid through antioxidant activity. This effect is clearly perceptible with the E2 isoform, but less so with E3 and even less so with E4.
- However, Leininger-Muller et al (82) showed that apo E is sensitive to attacks by free radicals, with the responses being isoform dependent. The E4 isoform is more sensitive than is the E3 isoform, which in turn is more sensitive than is the E2 isoform. An antioxidant such as EGb 761 protects apo E from oxidation in a similarly isoform-dependent way; the effect is seen most clearly with apo E4 (82).
- Ramassamy et al (33) established that another relation existed between the apo E genotype and lipoperoxidation in AD. They showed that the level of peroxidation in the brains of AD patients depended on the apo E genotype and was higher when the E4 allele was present. This discovery is important because it explains why previous studies sometimes found an increase and sometimes found no change in lipoperoxidation in the brains of AD patients. Ramassamy et al also showed that the level of peroxidation in the brains of AD patients is inversely proportional to the concentration of apo E, which confirms the hypothesis that apo E has a beneficial effect against lipoperoxidation and that the effect is more pronounced when the patient has no E4 allele. Ramassamy et al proved, in vitro, that EGb 761 effectively reduces the level of lipoperoxidation in the brains of AD patients.
Cardiovascular concerns
The heart, along with the brain and retina, have the most mitochondria and those three suffer first when energy demand exceeds supply.
Mitochondria and cardiovascular diseases—from pathophysiology to treatment (Gerasimos Siasos, et al, 2018) (bold font added for emphasis):
- Mitochondrial dysfunction is associated with the development of numerous cardiac diseases such as atherosclerosis, ischemia-reperfusion (I/R) injury, hypertension, diabetes, cardiac hypertrophy and heart failure (HF), due to the uncontrolled production of reactive oxygen species (ROS). Therefore, early control of mitochondrial dysfunction is a crucial step in the therapy of cardiac diseases.
Mitochondria and Heart Disease (Shaunrick Stoll, et al, 2017):
- Mitochondria play a key role in the normal functioning of the heart and in the pathogenesis and development of various types of heart disease. In addition, specific mitochondrial cardiomyopathies due to mutations in mitochondrial DNA have been identified. Increasing studies demonstrate that mitochondrial function has emerged as a therapeutic target in heart disease. This chapter addresses the recent studies of the role and the mechanism of mitochondria in the development of heart disease, and the progress in clinical diagnosis and treatments on a mitochondrial basis. Consequently, the aim of this chapter is to outline current knowledge about mitochondria in the heart disease.
Mitochondria-targeted agents: Future perspectives of mitochondrial pharmaceutics in cardiovascular diseases (Thekkuttuparambil Ananthanarayanan Ajith and Thankamani Gopinathan Jayakumar, 2014):
- Dysfunction of mitochondria increase the risk for a large number of human diseases, including cardiovascular diseases (CVDs). Heart failure (HF) following ischemic heart disease, infantile cardiomyopathy and cardiac hypertrophy associated with left ventricular dilations are some of the CVDs in which the role of mitochondrial oxidative stress has been reported.
Longevity
Chronological age is the number of years a person has been alive, while biological age refers to how old a person seems to be. Biological age is intrinsically associated with how healthy the mitochondria are. One of the hallmarks of aging is mitochondrial dysfunction caused by accumulation of damage, source: The Hallmarks of Aging (Carlos López-Otín et al, June 6, 2013).
Mitochondria: In Sickness and in Health (Jodi Nunnari and Anu Suomalainen, 2016) (bold font added for emphasis):
- Mitochondria perform diverse yet interconnected functions, producing ATP and many biosynthetic intermediates while also contributing to cellular stress responses such as autophagy and apoptosis. Mitochondria form a dynamic, interconnected network that is intimately integrated with other cellular compartments. In addition, mitochondrial functions extend beyond the boundaries of the cell and influence an organism’s physiology by regulating communication between cells and tissues. It is therefore not surprising that mitochondrial dysfunction has emerged as a key factor in a myriad of diseases, including neurodegenerative and metabolic disorders. We provide a current view of how mitochondrial functions impinge on health and disease.
This article, Mitochondria shown to trigger cell aging in reporting on the findings of this study Mitochondria are required for pro‐ageing features of the senescent phenotype (Clara Correia‐Melo, et al, 2016) (bold font added for emphasis)
- In a study, published today in the EMBO Journal and led by Dr João Passos at Newcastle University, they found that when mitochondria were eliminated from aging cells they became much more similar to younger cells. This experiment was able for the first time to conclusively prove that mitochondria are major triggers of cell aging.
Mitochondria and Aging (Christiaan Leeuwenburgh, et al, 2011)
- During the last two decades, interest relating to mitochondria in the field of aging has grown exponentially. Nowadays, it is known that mitochondria are more than just the power-houses of the cell. They participate in almost every aspect of metabolism.
Mitochondria, Oxidants, and Aging (Robert S. Balaban, et al, 2005) (bold font added for emphasis):
- For, although mitochondria are marvels of energy production, they also have another, less beneficial legacy in the cell. Increasingly, this other property, the continuous production of potentially harmful reactive oxygen species (ROS), has become a central focus of aging research. The purpose of this review… to evaluate to what degree the mitochondrial production of ROS and the cellular response to oxidative stress may be a major determinant of how we age.
Mitochondria and Aging (Chris Smelick, Aug 14, 2005) is not a published/peer reviewed study but an interesting article which says:
- Mitochondrial Theory of Aging: Does ROS Generation Initiate a Vicious Cycle?
- An unfortunate side effect of aerobic respiration in mitochondria is that the electrons donated to the ETC can often "leak out" and, rather than driving the creation of the pH gradient, can instead go on to form unstable molecules called reactive oxygen species (ROS). Unstable ROS are capable of damaging many types of cellular components, and it is thought that the damage that may accumulate over time from ROS generated from aerobic respiration may play a significant role in aging. Given that mitochondrial DNA exists in the inner matrix and this is in close proximity to the inner membrane where electrons can form unstable compounds, mtDNA has a relatively high chance of getting damaged by ROS. This entails mutations to mtDNA (or straighout deletions of many base-pairs) that can result in the manufacturing of mutant ETC proteins that, in turn, can lead to the leaking of more electrons and more ROS. This so called "vicious cycle" is hypothesized to play a critical role in the aging process according to the mitochondrial theory of aging.
- Evidence for Mitochondrial Dysfunction Being Causal in Aging
- There is a wealth of evidence that suggests that mitochondria are implicated in aging process and senescence. Specifically, loss of mitochondrial genome integrity is speculated to constitute. When the proofreading component of mitochondrial polymerase was knocked out in mice models, the mtDNA mutations that resulted caused a phenotype resembling premature aging (Larrson et al., 2004). Additionally, mtDNA mutations are found to accumulate with age in humans. Yet, it cannot be said that the mice phenotype literally is aging. It simply resembles aging. Similarly, the acculumation of mtDNA mutations might be the byproduct of a process more fundamental to bringing about aging, rather than actually causing aging. Only more experiments will determine the exact role of mitochondrial in the aging process.